Prioritizing the Health of MSM: Extragenital STD Screening Call-to-Action
The Gay Men's Health Equity Work Group developed a Call-to-Action and supplemental infographics encouraging improved STD screening of MSM, specifically of the throat and rectum.


Executive Summary
Though many sexually transmitted diseases (STDs) remain undiagnosed and unreported, 2016 was the third consecutive year in which national increases were seen in reported chlamydia, gonorrhea, and syphilis infections. Gay, bisexual, and other men who have sex with men (MSM) are disproportionately impacted by these STDs.1 STD screening of MSM, specifically of the throat and rectum, needs to improve. This is a call to action for health departments and medical providers to normalize extragenital STD screening, also known as 3-site testing.
Background
Total combined cases of chlamydia, gonorrhea, and syphilis reported in 2016 reached the highest number in 20 years – there were ~1.6 million chlamydia cases; 468,514 gonorrhea cases; and 27,814 primary and secondary (P&S) syphilis cases reported. The largest increase in cases from 2015 to 2016 occurred in gonorrhea (18.5%), followed by P&S syphilis (17.6%) and chlamydia (4.7%). MSM accounted for the majority of new P&S syphilis cases (80.6% of male cases with known gender of sex partner). Data from the STD Surveillance Network (SSuN) also suggest gonorrhea rates have increased among MSM for the last five years. 1 Antibiotic-resistant gonorrhea is also a concern and may be increasing among MSM. Syphilis rates are at levels not seen since 1992 and disproportionately impact Black and Latino gay men. 1 Gay, bisexual, and other men who have sex with men (MSM) continue to face the highest rates of syphilis and HIV co-infection. 1
Scope of the Problem
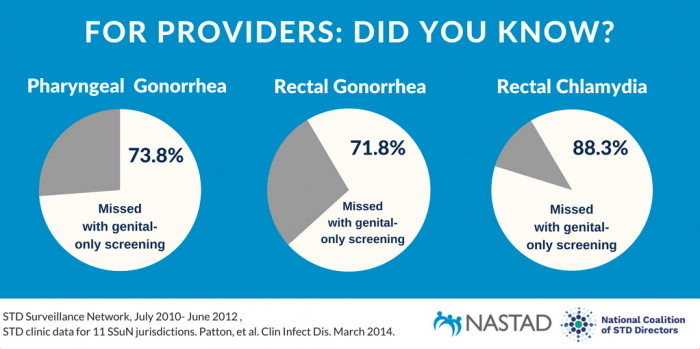
It has been well established that urethra only screening for chlamydia and gonorrhea in MSM misses most infections.2,3,4,5,6 The U.S. Centers for Disease Control & Prevention (CDC) recommends screening sexually active MSM at least annually for urethral and rectal chlamydia and for urethral, rectal and pharyngeal gonorrhea.7 Unfortunately, nucleic acid amplification tests (NAATs) have not been cleared by the Food and Drug Administration (FDA) for the diagnosis of extragenital chlamydia or gonorrhea. However, laboratories may validate their FDA-cleared NAATs for use on rectal and oropharyngeal specimens.8
In a national survey of US physicians, fewer than one-third routinely screened patients for STDs.9 In a large, urban HIV care clinic, extra-genital STD testing was low (29-32%) even though the frequency of syphilis testing was high (72%).10 HIV primary care providers lacked testing and treatment knowledge (25-32%) and cited lack of time (68%), discomfort with sexual history taking and genital exam (21%), and patient reluctance (39%) as barriers to increased STD testing.10 Even among STD clinics, extragenital STD screening was common, but many MSM were not tested.5
The Gay Men’s Health Equity Work Group offers these recommendations for extragenital STD screening to health departments, encouraging them to engage and collaborate with medical providers, laboratories, community-based organizations, and MSM themselves.
For resources to help implement these recommendations, please visit the NCSD extragenital webpage, which will be updated on an ongoing basis. NCSD and NASTAD and the National Network of STD Clinical Prevention Training Centers produced the MSM Sexual Health Standards of Care as a toolkit for providers to improve health services for gay, bisexual, and other MSM.
For full document and to view citations, click here.
Health Department Recommendations
Health Department Recommendations:
- Add anatomical site of chlamydia and gonorrhea infections to case report forms and surveillance summaries to ensure data are available to drive resource allocation.
- Prioritize and monitor STD screening of MSM in Ryan White care, especially of extragenital sites.10 Inclusion of non-syphilis STD measures in Ryan White care audits can be an effective monitoring tool for quality STD screening in those settings.
- Encourage health plans and provider groups to adopt quality improvement measures that include extragenital STD screening rates.
- Work with clinical settings and medical providers to:
- Screen for rectal chlamydia and gonorrhea infection in men who had receptive anal intercourse in the past year.
- Screen for pharyngeal gonorrhea infection in men who had receptive oral intercourse in the past year. CDC does not recommend testing for pharyngeal chlamydia infection, but most providers use combination tests for both chlamydia and gonorrhea.
- Promote MSM standards of care and regularly elicit risk-based sexual histories.5
- Implement effective strategies for improving screening rates in clinic settings, including standing orders for STD testing that includes extragenital specimens, and self-collection of rectal and pharyngeal specimens when a full exam is not feasible. 12,13,14
- Discuss and offer or refer for initiation of Pre-Exposure Prophylaxis (PrEP) for HIV-negative men with rectal chlamydia or gonorrhea.11
- Prioritize STD screening of sexually active MSM at least every 3 months – including extra-genital sites.
- Work with laboratories to
- Internally validate NAAT for diagnosis of extragenital chlamydia and gonorrhea infections.8 If this is not feasible, work with the Association of Public Health Laboratories (APHL) to identify and link clinical providers to laboratories that have already validated rectal and pharyngeal specimens for chlamydia and gonorrhea testing.
- Work with MSM-focused community-based organizations (CBOs) to
- Facilitate STD testing of MSM who may not be accessing testing elsewhere. Many CBOs offer HIV-only testing, which is a missed opportunity for identifying new STD infections.7
- Educate and promote extragenital testing as an essential sexual health practice.
- Encourage MSM constituents to demand regular risk-based extragenital STD screenings from their healthcare providers.
All images were developed as a supplement to the Call-to-Action. You can download all images and the full infographic above.




GMHE and Contact Info
The Gay Men’s Health Equity Work Group (GMHE) is a collaboration of members from the National Coalition of STD Directors and NASTAD with expertise in the sexual health of gay, bisexual, and other men who have sex with men.
With questions or comments, contact Desiree Smith, manager, health equity.